Health
Listed below are various topics which could possibly relate to your dog. To find out more, just click on the relevant topic.
- Why pets need to see the dentist too
Why pets need to see the dentist too
‘The Dentist will see you now…’
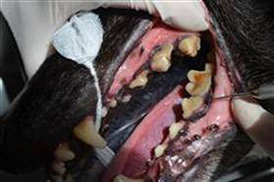 If that sentence made you feel sick to the stomach, thank you for continuing to read this far! Dental health is quite an easy thing to forget about in our pets, so it comes as no surprise that most recommendations for dental surgery happen at their annual health check or vaccination, which can often be a shock for pet owners.
If that sentence made you feel sick to the stomach, thank you for continuing to read this far! Dental health is quite an easy thing to forget about in our pets, so it comes as no surprise that most recommendations for dental surgery happen at their annual health check or vaccination, which can often be a shock for pet owners.How can I tell if my pet has a toothache?
As vets, we tend to see teeth in a much worse state than human dentists generally would; either because of the animal’s frustrating ability to hide that they are in pain, or even from their human’s own ‘dentist phobia’ – believe us, it happens! So keep an eye out for symptoms that your pet may be suffering from a toothache, such as:
- Loss of appetite
- Inability to eat
- Bad breath
- Broken teeth
- Lumps on the gums
- Facial swelling
- Rubbing their face or mouth
What happens if it’s not treated?
Now we’ve all heard of gingivitis but does anyone really take it that seriously? Gingivitis is where the tartar moves under the gum line, causing them to become inflamed, red and sore- ouch! If left untreated, it can develop into serious periodontal disease resulting in tooth loss, expensive extractions or infection affecting organs around the body.
How can it be prevented?
If the vet mentions that your pet could do with a scale and polish, don’t panic. This is the most common dental surgery we perform for pets. Just like in human dentistry, a scale and polish is performed to remove as much tartar and invisible plaque as possible to prevent any further and more serious dental disease from occurring. However, your pet will require a general anaesthetic, as they are far too wriggly to carry out even the most straight forward dentistry.
So although the thought of surgery mainly for preventative measures, like a scale and polish, may be a worrying thought, it can certainly save your pet a lot of discomfort and potentially serious health issues!
- Could your pet have diabetes?
Could your pet have diabetes?
 Just like in humans, diabetes is a growing concern for pets. Diabetes is caused by the pancreas not being able to produce enough insulin, or that the insulin produced is not being used correctly. Insulin allows glucose in the blood to enter cells, helping the body to function properly. Without this, it can be life threatening.
Just like in humans, diabetes is a growing concern for pets. Diabetes is caused by the pancreas not being able to produce enough insulin, or that the insulin produced is not being used correctly. Insulin allows glucose in the blood to enter cells, helping the body to function properly. Without this, it can be life threatening.What are the symptoms?
If your pet is showing any of the below signs, they could be at risk of having diabetes.
- Increased thirst or excessive drinking
- Increased urination or “accidents” in the house
- Change in appetite
- Sudden weight loss, despite increased hunger
- Thin or dull hair
- Lethargy or weakness
- Vomiting
- Cloudy eyes or blindness
Like all illnesses, the earlier diabetes is diagnosed and treated, the better. There are estimated to be half a million undiagnosed diabetic people in the UK – imagine how many pets may also be at risk! Once diagnosed, it can be an easy to manage condition and your pet can lead a happy, healthy life.
It is thought that obese pets and female dogs are at greater risk of diabetes later in life, and some breeds can actually be predisposed to the condition. To help lower the chances of your pet developing diabetes, we recommend they maintain a healthy lifestyle with plenty of exercise and a suitable diet.
- 7 Signs of Ear Disease
7 Signs of Ear Disease
 Does your dog shake their head a lot? Or have you noticed a less than pleasant smell coming from their ears? This could be a sign of ear disease. Ear infections and problems are some of the most common issues we treat as vets, particularly in dogs with long, floppy ears.
Does your dog shake their head a lot? Or have you noticed a less than pleasant smell coming from their ears? This could be a sign of ear disease. Ear infections and problems are some of the most common issues we treat as vets, particularly in dogs with long, floppy ears.What are the signs of ear disease?...
- Odour from the ears
- Discharge in the ears
- Scratching or rubbing at the ears or head
- Shaking of the head or tilting of the head
- Redness inside the ears
- Pain around the ears
- Irritable or depressed behaviour
How to prevent ear disease
Check your pet’s ears on a regular basis to make sure they are clean, healthy looking and smell normal. We recommend regular cleaning using a veterinary recommended product, particularly if your dog swims a lot, has the aforementioned floppy ears or if your breed of dog is more prone to ear disease such as cocker spaniels, golden retrievers and schnauzers. Make sure ears are thoroughly dried after having a bath or swimming and trim away any excess hair around the ears to encourage more air flow.
If your pet is showing any of the above symptoms, don’t delay, book in to see the vet now.
- The Dangers of Giant Hogweed
The Dangers of Giant Hogweed
 A woman whose dog suffered horrific burns after it sniffed toxic Giant Hogweed has warned other pet owners of its dangers.
A woman whose dog suffered horrific burns after it sniffed toxic Giant Hogweed has warned other pet owners of its dangers.Joanne Boardman, 47, had taken her beloved rescue dog on her daily walk through some fields and allotments near her home in Graystones, Sheffield. But within hours of returning, eight-year-old Ellie the Great Dane was covered in sore blisters and whimpering in pain.
Joanne, of Graystones, Sheffield, said: "At first I noticed that Ellie had some little marks on her nose which looked like scratches, but I didn't really think much about it. The following day it blistered up really badly when she went out in the sun. It went from nothing to these horrible blisters. Ellie was in a lot of pain and she couldn't ignore it. It's on her nose - the most sensitive place. She is such a friendly, happy dog normally and this had a massive impact on her - she went really quiet and just wasn't happy at all. I was really worried and I didn't have a clue what to do, so I took her to the vets. When I first took her in, they thought she just had a skin condition. It wasn't until I posted some pictures on Facebook and a few of my friends said it could be Giant Hogweed that we realised what it was."
Giant Hogweed contains toxic components which, if touched, make skin extremely sensitive to sunlight meaning it can burn and blister easily. The plant, which can grow up to 3.5m tall, affects animals as well as humans and can cause severe burns, particularly in summer months when UV rays are strongest.
After staff at Park Veterinary Hospital realised what had caused Ellie's burns, they gave her painkillers and prescribed a course of antibiotics to stop the open blisters becoming infected.
Four weeks on, her wounds have begun to heal but the fur on her muzzle has been burned away and the skin underneath left red and scarred.
Joanne has been washing the area with salt water regularly and applying sun block so Ellie can still play outside because her skin is so sensitive. "I think Ellie must have come into contact with the sap in one of the allotments. People walk their dogs there all the time. I want people to know about hogweed and be aware that it's out there, because it's really dangerous. Something like this can have a devastating effect on animals as well as humans. It's just horrible to see a pet in so much pain."
Vet Carmel Stanford, who treated Ellie at Park Veterinary Hospital, said: "Ellie's nose was horrendously inflamed when Joanne brought her in. "It looked incredibly sore and the whole experience was very traumatic for the dog. When I realised it was Giant Hogweed I was really worried. It was also a really difficult area to treat because dogs like to sniff around, and obviously it was difficult when Ellie was eating. Luckily, it has healed up well. Dog walkers need to make sure they avoid this plant at all costs - even the smallest amount can cause severe burns."
Reports of injuries following contact with Giant Hogweed have drastically increased over the past month as UV rays are strongest in summer. As a result, affected skin is particularly sensitive and more prone to burns and blisters.
Hogweed, which is from Central Asia, is thought to have been brought to Britain in 1893 and now grows in parks, woods and on riverbanks around the country. Its leaves, stems, roots, flowers and seeds contain toxic components which can be transferred by contact and make exposed skin extremely sensitive to sunlight.
Burns are particularly severe in the summer months as UV rays, which cause affected skin to blister, are particularly strong.
With thanks to The Daily Mail.
- Pet Passports
Pet Passports
Please visit the official government website and search for 'Pet Passports' to check you have covered all requirements for the country you are visiting.
- Fleas and Ticks
'Tick-ing' Time Bombs
 Fleas and ticks are unpleasant in their own right, but they are also a threat to the health of your pet and your family. So make sure you protect everyone in your household from these nasty critters by using prevention treatments on a regular basis. Both bugs have been shown to spread a number of diseases in pets and humans, some of which can be a serious health risk such as:
Fleas and ticks are unpleasant in their own right, but they are also a threat to the health of your pet and your family. So make sure you protect everyone in your household from these nasty critters by using prevention treatments on a regular basis. Both bugs have been shown to spread a number of diseases in pets and humans, some of which can be a serious health risk such as:- Cat scratch fever (bartonellosis) – may cause fever, headache, fatigue and poor appetite in humans
- Rickettsia felis – causing fever, headache, muscle pain and rash in humans
- The flea tape-worm (Dipylidium caninum)
- Lyme disease (borreliosis)- a bacterial disease affecting dogs, horses and people
- In dogs it may cause lameness, fever, anorexia, lethargy, swollen joints and rarely kidney failure
- In humans it may cause a rash and flu-like symptoms, but may eventually produce abnormalities in the joints, heart and nervous system
- Babesiosis - caused by a microscopic parasite that invades red blood cells has also been shown to be carried by UK ticks. The disease can manifest with high temperature, increased respiratory rate, muscle tremors, anaemia, jaundice, and weight loss.
Animals with flea infestations frequently develop flea allergic dermatitis (FAD); caused by a persistent intense irritation of the skin leading to significant distress, scratching, chewing, skin damage, hair loss, eruptions and infections. Heavy infestations especially in puppies and kittens may lead to iron-deficiency anaemia.
Speak to your Vet to find out which product would be most suitable for your pet.
From the Highcroft Vet Group blog.
- Recognising the Symptoms of Pyothorax
Recognising the Symptoms of Pyothorax
Know Your Own Dog
It can’t be stressed enough, if you really know your own dog, all those tiny, subtle aspects of his everyday character, then you know when he’s just “not himself” and in my experience this is usually cause for concern! There may be exceptions to this rule but in my 21 years of having dogs who we have loved dearly and treated as members of our family, if they can possibly carry on as normal, doing what they always do, then they will – by the time they are acting differently and not being their normal selves then they are probably suffering from something that requires immediate veterinary attention! And it’s at this point that you really need to be persistent and insistent with your vet who may think your dog appears to be fine and you are just being over-anxious!!
I can illustrate this with our 4 year old Italian Spinone, Bracket, who has just undergone major chest surgery at a referral veterinary hospital where he spent 11 days. No doubt, even with immediate intervention by our vets he would have needed treatment requiring a stay with them perhaps for a few days. However, because to them he appeared to be lively and had normal vital signs, temperature, heart rate etc., an infection in his chest cavity was allowed to brew for another 2 weeks before it was taken seriously.
Of course, because I know him so well, I knew there was something very wrong, but up to this point I have always found our local vets to be excellent and have put my trust in them. Consequently I just went along with what they were saying which at first was “oh he’s probably done something a bit silly and given himself a knock and now he’s a bit sore”. He was given Rimadyl and sent home.
I should explain at this point that the only symptoms I could describe to the vets, apart from “he’s not his normal self” were that he was having trouble getting comfortable when he settled and that his breathing rate was rather fast.
On subsequent visits (there were five in all) his temperature started to rise and my observations about his breathing became more serious – there were times when, even though he was asleep, he was taking 90 shallow breaths per minute! Two different vets listened to his chest at each visit but were not really worried by what they could hear. One of the vets started going down the route of his increased breathing rate being caused by the fact that he was in pain and started to suspect pancreatitis. This gave rise to further, unnecessary tests. On the fourth visit it was said that his chest sounded a “little rough” and he was given anti-biotics by the other vet who didn’t agree with the pancreatitis theory.
Not until the fifth visit did they x-ray his chest. As soon as they saw the x-ray I think they realised their mistakes and Bracket was immediately booked into a referral centre where he could get expert help. His chest was so full of fluid that nothing was visible on the x-ray.
So, off we went on the hour and a quarter trip to Oakwood referrals in Cheshire. He spent the next 11 days there. The diagnosis was Pyothorax (pus in the chest cavity). The hope was to avoid surgery so large chest drains were put in place to drain off the fluid which they had established was full of pus and infection. However, 48 hours later the specialist had to perform surgery because the chest drains had become blocked with all the solid matter and the infection was being pushed into other tissues outside of his chest cavity. This, of course, means a much longer recovery time with all the problems associated with a large surgery wound.
So, the point of this article is twofold:
1) to stress that if you are close to your dog and really know him or her, then you must trust your instincts and push your vet to accept that there really is something wrong even though, to the vet, your dog may appear to be quite normal, and
2) if your dog’s breathing is more rapid than usual (it’s a good idea to get familiar with what is normal for your dog when he’s completely at rest) and he’s not his normal self, i.e. a bit less energy, a bit uncomfortable etc., even though he’s still eager for food and walks, then there could be fluid build up in his chest.
Apparently, Pyothorax can be caused by something as simple as inhaling a grass seed! It can also be caused by a penetrating bite wound that has long since healed and been forgotten about or by normal bacteria circulating in the blood. In Bracket’s case I am told there was no “focal point to the infection” and so is likely to have been caused by bacteria. Apparently some animals (and people for that matter) seem to be predisposed to this. Although there is no published evidence as yet, it seems that dogs who have an underactive thyroid gland (which Bracket does) may fall into this category. Also, he did have a severe bite to his chest when he was attacked as a 13 week old puppy, that was 4 years ago, but although the specialist declared that it would be unusual if that was the cause after all this time, she didn’t rule it out! The following link outlines the condition: Pyothorax in Dogs.
So, at this point in time Bracket is awaiting the removal of his staples and he is putting up with severely restricted activity! His two pals, Chisel, another Spinone and Daphne, the Daneline Rescue Great Dane are being very careful with him, bless them! Unfortunately Bracket doesn’t seem to feel the same need to be careful with them!! As ever, if you didn’t know, you would think he was as right as rain!!
Julie Stanford
- Summer Hazards
Summer Hazards
BBQ’s
Giving left overs to your pet is a bad habit and can result in causing upset stomachs or even worse pancreatitis which can be a life threating condition.
Owners should be aware of foods such as grapes, onions and raisins are highly toxic to dogs and should not be given under any circumstances.
Foreign bodies
Are also an issue at this time of year due to food waste being left around the garden which animals are prone to pick up. Corn on the cob is a very common cause of an intestinal foreign body in dogs as these are unable to be digested, and these are also the cause of choking.
Foods with bones such as chicken legs/wings are very dangerous for our pets due to them splintering the gastrointestinal tract or bowel. Toothpicks and skewers are also a hazard which can result in the same outcome.
Buzz off
Stings from wasps and bees are a common summer hazard. These can cause major discomfort and distress to your pet.
If your pet is stung apply a cold compress to the area to help with the swelling. Pets should be seen by a vet especially if they are showing signs of breathing difficulties.
Ticks
These are present throughout the year, however they become more common in the summer months due to the increased time spent outdoors especially in woodlands and thick grass areas.
To prepare your pet getting these unwelcome friends, regular checks together with ensuring their tick treatment is up to date can reduce the chances of them attaching to your pet.
The sun has got his hat on!!
Do you know noses and ears of your pet have a higher chance of getting sunburnt? Applying sun cream to these areas can prevent this from occurring. White coated pets suffer particularly from this so restricting their time in the sun especially at the hottest time of the day can prevent this from occurring.
Restricting your dog walks to mornings or evenings when the temperature is at its coolest can make this more comfortable for your dog and help prevent over heating.
Closing animals in vehicles and conservatories should also be avoided at all costs, as these areas can become extremely hot which may result in your pet suffering from heat stroke, dehydration or even death.
If for some reason your pet needs to be left in these environments, ensure a window is left open and they have access to plenty of clean fresh water which can reduce the chances of these reactions occurring.
If your pet has a long thick coat, regular combing will remove excess hair and in turn reduce their body temperature.
Signs shown for dehydration:
- Lethargy
- Decreased urination
- Dry gums
- Sunken eyes
If any of the above signs are shown, a cool towel should be placed over your pet and then seek veterinary attention as quickly as possible.
Did you know a dog’s pant helps cool them down? Other ways to help your pet cool down could include:
- Fans
- Ice treats
- Sprinklers
This information has been taken from Dowding Vets Gainsborough newsletter.
- Dogs Die in Hot Cars!
Dogs Die in Hot Cars!
 Don't leave your dog alone in a car. When it’s 22°C/72°F outside, the temperature inside a car can reach 47°C/117°F within 60 minutes.
Don't leave your dog alone in a car. When it’s 22°C/72°F outside, the temperature inside a car can reach 47°C/117°F within 60 minutes.Dogs pant to keep cool. In hot, stuffy cars dogs can’t cool down - leaving a window open or a sunshield on windscreens won’t keep your car cool enough.
If you see a dog in a car on a warm day, call the Police on 999. If the police are unable to attend, please call the 24-hour cruelty line on 0300 1234 999.
Heatstroke - early warning signs
Heatstroke can be fatal. Some dogs are more prone than others:
- dogs with short snouts
- fatter/muscley dogs
- long-haired breeds
- old/young dogs
- dogs with certain diseases/on certain medication
Heatstroke develops when dogs can’t reduce their body temperature. Symptoms include:
- heavy panting
- profuse salivation
- rapid pulse
- very red gums/tongue
- lethargy
- lack of coordination
- reluctance/inability to rise after collapsing
- vomiting
- diarrhoea
- loss of consciousness
Heatstroke - first aid
Act quickly, heatstroke can be fatal! If dogs show any signs of heatstroke, move them to a shaded, cool area. Ring your vet immediately.
Urgently, gradually lower their body temperature:
- Immediately douse them with cool (not cold) water, to avoid shock – you could use a shower, or spray and place them in the breeze of a fan
- Let them drink small amounts of cool water
- Continue dousing until their breathing settles – never cool dogs so much that they begin shivering
Once your dog is cool, immediately go to the vet.
Warm weather tips
- Your dog must always be able to move into a cooler, ventilated environment
- Never leave dogs alone in cars, glass conservatories or caravans even if it’s cloudy
- If you do leave dogs outside, you must provide a cool shady spot where they can escape from the sun
- Always provide good supplies of drinking water, in a weighted bowl that can’t be knocked over. Carry water with you on hot days.
- Groom dogs regularly to get rid of excess hair. Give long-coated breeds a haircut at the start of summer.
- Never allow dogs to exercise excessively in hot weather
- Pavements and roads can burn their pads.
- Dogs can get sunburned – particularly those with light-coloured noses/fur on their ears. Ask your vet for advice on pet-safe sunscreen.
- Leptospirosis Outbreak - URGENT WARNING TO ALL DOG OWNERS
Leptospirosis Outbreak
Please be aware that we have seen a number of cases of Leptospirosis (also known as Weil’s disease) at our surgeries during December. Until now, this disease has been very rare in vaccinated dogs. However, as we have seen a number of cases recently in vaccinated dogs, we suspect that a new strain of Leptospirosis bacteria is emerging in this area, one that the classical vaccination does not protect against.
Leptospirosis is a serious bacterial infection which can cause liver and kidney failure and can be fatal if not treated promptly. Spread by rats and contracted from areas of stagnant water, it is also possible for humans to contract Leptospirosis, particularly children or people with a poor immune system.
All of the cases we have seen so far have been in dogs living or exercising in the countryside to the South of Bristol.
How can I protect my dog?
Highcroft has acted immediately by sourcing the L4 Leptospirosis vaccine, which gives protection against more strains than the traditional vaccine, and we urge all vaccinated dogs to have this additional protection. Please contact your nearest surgery now. We have also changed our vaccination protocol for dogs to limit the risk of contracting this disease in the future.
- Kennel Cough
Kennel Cough
KENNEL COUGH: The UK’s most widespread infection disease of dogs. Persistent, unpleasant - and really easy to catch.
Kennel cough is a dry, retching, 'honking' cough that affects dogs of all ages. It can last for weeks, and is very hard to treat effectively. And yet, last year, an estimated 40,000 cases were seen by vets in the UK alone.
WHAT IS KENNEL COUGH AND WHAT CAN IT DO?
Kennel cough – also known as infectious tracheobronchitis – is a complex, highly infectious respiratory disease which circulates in the dog population all year round. Although a range of bugs can be involved, the two most likely triggers are both common and widespread: a bacterium called Bordetella Bronchiseptica and canine parainfluenza virus.
Once exposed to infection, it takes 3 to 10 days before the disease is seen – usually a persistent honking cough and fever. More rarely, serious cases can result in pneumonia and even death, particularly in puppies or those with a weaker constitution.
Depending on the severity of the disease, it can last from a few days to several weeks. But even after the coughing has stopped, your dog can remain infectious for three months or more.
IS YOUR DOG AT RISK?
Every dog is it risk, however healthy. Comprehensive protection against the most important causes is not normally included in routine annual vaccinations and any infected dog can pass the disease on.
Despite the name, a recent survey suggests that less than half of outbreaks arrays in kennels. Your pet is at least as likely to encounter the disease in common circumstances such as:
- The park
- The street
- At dog shows
- In training classes
- From next door's pet
Any place, in other words, where dogs meet.
WHAT'S THE TREATMENT?
Since kennel cough is called by both bacteria and viruses, antibiotics can sometimes help reduce disease duration but often have little impact on symptoms.
Other therapies such as anti-inflammatory drugs and cough suppressant are often only minimally effective and should be used under veterinary advice.
Unfortunately, by the time your dog has started coughing, the disease has already damaged its respiratory system.
As with any serious disease, prevention is always better than cure. Effective intranasal vaccines are available against the most significant causes and can be administered routinely alongside your pet's normal annual boosters.
For more information about vaccination against kennel cough, visit www.future-of-vaccination.co.uk.
- Winter tips for your dog
Winter tips for your dog
Here are a few tips to keep your dog happy and healthy over this festive time.
During the winter months there are many holidays where we celebrate by visiting or being visited by friends and family. This time can be both exciting and stressful, not only for us but our pets as well.
Dogs often enjoy having new faces to interact with; however this can lead to over excitement during their visit. To help reduce the stress and excitement for visitors and your pets, provide areas where dogs can go without visitor interaction so dogs that wish to avoid your guests may escape to, or a room to place your dog to allow your guests to enter without being mugged especially guests who are very young or elderly.
Provide extra distractions for your dog with chews, toys and long walks before your guests arrive. Provide calming aids including items like Adaptil, a plug-in diffuser (looks like an air freshener) designed to help reduce the feelings of stress and anxiety in your dog, reducing unwanted behaviours.
Winter and Christmas hazards
Christmas decorations
Christmas lights can be very dangerous if chewed by the dog or tangled up by the cat. Make sure your Christmas tree is stable and secure, cats love pawing at dangling objects and a Christmas tree bauble is too tempting for them to leave alone! A falling tree could cause major damage.
Freezing weather conditions
If walking dogs in freezing weather or rain is unavoidable, make sure you dry them off as soon as possible with a towel or hair dryer on a low setting held at some distance from your dog.
Safety at night
The nights are now drawing in and often we have to take our dogs out in the dark at night. Please make sure your cats and dogs are visible when out after dark with reflective collars, leads and jackets. If you let your dog off the lead, LED lights can be bought to add to their collars so you can see them when they go off into the dark.
Fireworks
Unfortunately the fireworks season is not quite over with yet so please keep your pets safe. For more information call into the surgery or give us a call.
Antifreeze
This is poisonous to animals especially cats, if you suspect your animal has ingested antifreeze, contact your vet immediately.
Here is a list of poisonous foods for dogs:
- Potatoes with green skins
- Sprouts
- Rhubarb Leaves
- Chocolate
- Caffeine
- Alcohol
- Avocado
- Grapes
- Raisins
- Currants
- Sultanas
- Macadamia Nuts
- Yeast Dough
- Xylitol
- Corn on the cob
- Onions
- Garlic
- Mushrooms
- Apple Seeds
Please contact your vet urgently if any of the above foods are consumed.
- Fireworks
Fireworks
“Remember, remember, the fifth of November!”. We all look forward to firework night; however it is easy to forget how stressful the event is for our pets. A recent study conducted by the University of Bristol showed that “almost half of owners in the structured interview reported that their dog showed at least one behavioural sign typical of fear when exposed to noises”. Some cases can become extreme and create a huge impact on owners’ lives.
Signs of fear:
- Trembling and shaking
- Clinging to owners
- Barking excessively
- Cowering and hiding
- Trying to run away
- Soiling the house
- Pacing and panting
- Refusing to eat
Top ten tips:
- Provide a den or hiding place for your pet whilst the fireworks are going off. Place somewhere they usually like to hide and line with familiar smelling towels or blankets. Cover the top with a blanket if possible. These should be prepared at least 3 weeks before the event so they have a chance to get used to it.
- Consider using pheromone diffusers or sprays such as Pet Remedy, as close to the den as possible. Another alternative is Zylkene or Kalm Aid supplements, which is an oral treatment to help with anxiety. Speak to one of our vets or nurses for more advice on any of these products or if you feel your pet needs something “stronger”. These will also need to be started well in advance of the event in order to be effective.
- Ignore fearful behaviour. Pets can pick up on their owner’s anxiety which can make the problem worse.
- Walk your dog early or well before the fireworks are due to start- this will also help to tire them out!
- Ensure all windows, doors and cat flaps remain closed to prevent pets escaping. It may be worth updating their identification, just in case they try to run away at any point.
- Make sure your cats have access to enough litter trays, especially if you’re keeping them indoors. Cats often get cystitis at times of stress.
- Don’t forget your small furries! Rabbits, guinea pigs or other outdoor pets should be brought inside wherever possible, or at least cover their hutch to help reduce the noise and light.
- Provide distractions, such as new toys or treats. Plus draw your curtains and turn on the TV to mask the noise.
- Try not to leave your pets alone when the fireworks are going off.
- DO NOT punish your pet for any fearful behaviour! This will only make your pet more distressed and worse in the future.
- Firework Precautions
Firework Precautions
Not every dog is frightened by fireworks, BUT many are absolutely terrified and who would want 50-75Kg of demented, terrified pooch?!
Here are a few points to consider. Please read them and choose whatever is best for your situation.
- Minimise the effect by walking earlier in the evening before the displays start
- Close the curtains and consider playing background music
- Provide a "safe place" with familiar objects or blankets
- Ensure that your dog can be identified if he runs away
- Start your preparations early, especially if you are considering D.A.P. (Dog Appeasing Pheromone)
- Good all round advice from the BANES dog warden
- General advice from RSPCA with a chance to support a bill that is currently before parliament and Blue Cross
- Also some common sense advice from a vet
Dog Appeasing Pheromone (D.A.P.) mimics the properties of the natural pheromones of the lactating female.
Remember each dog might react differently to fireworks and any of these treatments. Daneline recommends that you seek advice from your Vet and accepts no liability for the information given here.
- K.Laser Therapy for dogs
K.Laser Therapy for dogs
THERAPEUTIC EFFECTS
The painless application of laser energy promotes increased circulation by drawing oxygen and nutrients to the effected area. This creates an optimum healing environment reducing inflammation, swelling, muscle spasm, stiffness and pain. As the injured area returns to normal, pain is relieved and function is restored.
CELLULAR EFFECTS
During treatment, infrared laser light interacts with tissues at the cellular level. Increased metabolic activity within the cell stimulates the transport of nutrients across the cell membrane initiating increased production of cellular energy (ATP). This leads to a cascade of beneficial events promoting the acceleration of the healing process and reduced pain.
REINTRODUCTION TO ACTIVITY
While your pet may exhibit renewed energy after the first treatment, consult your veterinarian before your pet returns to full activity. A gradual introduction of activity may be suggested to ensure the patient does not aggravate the condition.
WHAT TO EXPECT
There is no patient sedation or restraint required and the experience is usually pleasant and comforting to them. K-Laser Therapy treatments are cumulative in nature. The length and frequency of treatments varies with your pet's condition. Even though improvements may be seen after the first visit, most patients require several treatments (3 to 8) for greatest benefit, and we recommend a multi-visit treatment plan. Most sites require 2 to 8 minutes per treatment.
A sample treatment schedule is as follows:
- Every other day for one week (3 total)
- Twice the second week (2 total)
- Once the third week (1 total)
- Boosters as needed
Your veterinarian will recommend a treatment plan specific to your pet's condition.
WHAT IS LASER THERAPY
Class IV K-Lasers deliver specific red and near-infrared wavelengths of laser light to induce a therapeutic effect within the body. These include increased circulation, decreased swelling, reduction of pain and enhanced tissue repair. Laser therapy has been used in Europe since the 1970s and was cleared by the United States Food and Drug Administration in 2002. K-Laser has become the preferred choice for thousands of animal and human practitioners worldwide.
Numerous Studies show that Laser Therapy can help with:
- Osteoarthritis
- Joint Pain
- Tendinopathies
- Edema and Congestion
- Ligament Sprains
- Muscle Strains
- Puncture Wounds
- Post-Traumatic
- Injury
- Post-Surgical Pain
- Neck and Back Pain
- Hip Dysplasia
- Burns
- Chronic Wounds
- Rehabilitation
- Post-Orthopedic
- Surgical Recovery
- Taking your dog abroad - some important information
Taking your dog abroad
Summer holidays are coming and we know some of you will be taking your dogs abroad. Please be aware of the potentially fatal Leishmaniasis disease. This is transmitted via a bite from the female sand fly whose habitat is not in sand as the name suggests. There are some precautions you can take to radically reduce the chances of your dog contracting this awful disease. Use Advantix spot on drops before you go. Buy a Scalibor collar and put it on 2/3 weeks before travelling (take it off when or if your dog goes swimming).Keep your dog indoors half an hour before sunset until half an hour after sunrise before allowing him/her outside. An extra precaution is to vaccinate with a product that includes CaniLeish (this does not eliminate the risk but it does help with reducing the risk). On your return contact your vet about the appropriate timing for a blood test. We do not want to alarm you but better to have the information before rather than after the horse has bolted! The following is an informative article.
Canine Leishmaniasis - the facts
by Dr Bob Killick-Kendrick PhD, DSc, FIBiol
Reading the many articles on the dangers of British dogs catching leishmaniasis when they are on a Mediterranean holiday, I can imagine dozens of owners rushing to their telephones to cancel plans for holidays with their dogs. But it is not quite as bad as it seems, there are ways the risk can be minimised. After all, there are lots of healthy dogs all round the Mediterranean. In France, where I now live, there are more dogs per head of the population than in the UK. This is in spite of the fact that leishmaniasis is common in many places. So what exactly causes canine leishmaniasis, how does a dog get infected and what can dog owners do to protect their pets?
The cause is a microscopic parasite that lives inside cells of the blood and internal organs. There are many species of these parasites all classified under the name Leishmania (after a famous Scottish doctor - Sir William Leishman - who discovered a species which causes epidemics in people in India). Most of these parasites have evolved in wild animals. They are generally pretty well adapted to these hosts and don't cause them any trouble. But if they get into the wrong host - like our dog- they can be dangerous. All of them are transmitted by the females of small blood sucking insects - sand flies - that first pick up an infection by feeding on an animal carrying the parasite. Like mosquitoes, sand flies need the protein in the blood to make eggs. In the stomach of the fly, the parasites keep dividing until they fill all the available space. Then, when the female takes another blood meal, she deposits some of the parasites into the skin of the unlucky individual and the cycle is completed. But many dogs bitten by an infected sand fly never get clinical leishmaniasis: they are able to control the parasite with their immune system. This depends on their genes and many vets think some breeds are more likely to get the disease than others.
To give the full picture, I ought to say something about sand flies. They are small two-winged insects - about 3mm long - that breed in damp soil rich in organic material. They are active from dusk to dawn and you can be bitten without knowing the culprit. You don't hear them when they come to bite and it's quite likely you won't know what caused the itchy spot the next day. If you do see one, it's easy to know it is a sand fly. They hold their wings up above the body, they are hairy, and they hop around as they are making up their minds where to bite. Leishmaniasis is not endemic where there are no sand flies. One species of Leishmania (L.infanta) infects dogs in countries bordering the Mediterranean, plus Portugal, many Latin American countries, parts of the USA, West Africa, Sudan, much of the Middle East, Central Asia and western China. British dog owners are, of course, more likely to take their pets to southern Europe than the more exotic places, so the rest of this article concerns transmission only around the Mediterranean and in Portugal.
Of course, if you take your dog to a place where there are no sand flies at all, there's no problem. But some popular holiday places are dangerous. In Portugal, there are hot spots in the Lisbon Metropolitan Region, the Evora district and Alijo, Alto-Douro. In Spain, the south is particularly risky, especially Salamanca, Granada, Jaen, Valencia, Murcia, Catalonia, the Northern Madrid area and the islands of Mallorca and Ibiza. In France, the most popular country for British holiday makers, your dog should be safe in a strip along the north (Brittany, Normandy and Picardy) and another down the eastern border north of Provence (Ardennes, Champagne, Lorraine and Franche-Comte); other parts of France are more or less dangerous. Most of Italy, all of Greece, and the islands of Cyprus, Malta, Gozo, Sicily, Sardinia and Corsica are risky.
But do not despair! It is safe to take your dog anywhere in southern Europe from the end of October to May when sand flies are hibernating as larvae in damp soil. Up to the end of May there's no real risk but, as summer gets into full swing, the chances of being bitten by an infected sand fly increase until late August and into September which is the time of greatest danger. All right! You don't want to go on holiday from October to May; you want to go when there's lots of sunshine. There's no magic pill or vaccine yet on the market to protect your dog from leishmaniasis. But there are ways you can reduce the danger to about the same level as having a fatal accident while driving from the English Channel port to the Mediterranean on French roads.
The best protection for dogs against sand fly bites is a plastic collar called Scalibor which is marketed in two sizes. Scalibor is a depot of the insecticide deltamethrin. This is insoluble in water (so dogs can swim while wearing the collar) but is soluble in the oils of the dog's skin. Friction between the collar and the neck of the dog releases tiny amounts of deltamethrin which are absorbed by the oils and spread over the body of the dog. Complete cover takes about 10-14 days. Scientific studies in France, Spain, Brazil and Iran have shown that Scalibor will protect a dog from well over 90% of sand fly bites for more than six months. In southern Europe that's a complete sand fly season. Field studies in Italy and elsewhere have shown dogs wearing Scalibor are very much less likely to catch leishmaniasis than dogs without the collar. One problem is that if you shampoo your dog, with a detergent shampoo, some of the skin oils are removed and, after Scalibor is replaced, it will take a few before the maximum level of protection is regained. But the manufacturers thought of that and are now beginning to market a Scalibor shampoo with enough deltamethrin in it to keep up the protection. The collar gives dog owners a bonus: it's also very good for protecting dogs from tick bites. And it is environmentally friendly because it targets only insects and ticks coming to bite a dog.
How do you know that, while sunbathing on the beach, your dog won't be bitten by a Leishmania-carrying sand fly? I can answer that question. Your dog won't be bitten dog while you're getting sunburned because there aren't any sand flies on the beach. It is not their habitat. Don't be misled by the name: many species are a sort of sandy colour and some live in sandy deserts but they have nothing to do with beaches. And if they were on the beach, they wouldn't bite your dog while you're sunbathing. They hate the heat and, during the day, they are tucked away in cool moist resting places like cellars or cracks in walls and they don't come out to attack until twilight. Sand flies of southern Europe begin biting as the sun goes down and carry on until dawn. Interestingly most of them bite outdoors, not inside houses, so it's a good idea to keep your dog indoors from dusk to dawn.
At the time of going to press OUR DOGS has received information from an official source that the Scalibor collar has been authorised in the UK which means that it should be available from veterinary surgeons. Because the availability of the collar is at its early stage it may be necessary for the vets to pressurise their pharmaceutical suppliers to obtain supplies but if enough travellers demand the product it should be forthcoming.
If your dog is going on holiday to a place in southern Europe where there is leishmaniasis, order a collar in plenty of time, put it on your pet two weeks before he sets a paw on the Continental mainland. This will reduce the risk to an acceptable level; but nobody can guarantee 100% protection against any disease. A UK dog owner must realise that, if a dog has been in a leishmaniasis endemic area in the summer, even if it was wearing Scalibor, there is a very faint possibility that the pet could have become infected. The time from a sand fly bite to the first clinical signs of leishmaniasis is usually around four to seven months but can occasionally be longer. Common early signs are loss of hair, especially round the eyes, skin sores, and loss of weight, but even experienced vets often find it difficult to diagnose canine leishmaniasis simply by a clinical examination. If a dog falls ill during the year after its return to the UK, it should be taken to a vet with a request for a blood test to check for leishmaniasis. This can be done in the Veterinary Faculty of Liverpool University.
If your vet doesn't know what you're talking about (he has probably never seen a case), suggest he looks at the website www.leishmaniasis.info where he will find all he needs to know about the clinical signs of canine leishmaniasis, how to make the diagnosis and how to treat his patient. There are also answers to the questions most frequently asked by dog owners.
Bob Killick-Kendrick PhD, DSc. FIBiol is an eminent parisitologist who has studied Canine Leishmaniasis for thirty based at Imperial College, London where he is Senior Research Investigator. He is also on the World Health Organisation expert panel on Canine Leishmaniasis an is a consultant to Intervet International which is responsible for developing the Scalibor collar.
- Dangerous and Toxic Foods For Dogs
Dangerous and Toxic Foods For Dogs
Please be aware of toxic and dangerous foods found mainly in your kitchen! Here is a list of foods that if ingested are toxic and can be fatal to dogs. To find more detailed information on each one, please use the internet. To be on safe side, feed your dogs only food made for dogs.
- Grapes
- Raisins
- Sultanas
- Currants
- Baby foods can contain onion powder
- Macadamia nuts
- Walnuts
- Uncooked yeast dough
- Xilitol, sugar free sweetner found in in chewing gum and sweets
- Fruit pits and seeds
- Rotten/mouldy foods
- Junk food
- Potatoes with green skins
- Sprouts
- Rhubarb Leaves
- Chocolate
- Caffeine
- Alcohol
- Avocado
- Xylitol
- Corn on the cob
- Onions, cooked or raw
- Garlic
- Mushrooms
- Apple Seeds
- Flea Treatments
Flea Treatments
The Life Cycle of the Flea
When choosing which flea treatment is suitable for you, it is important to know a little about the life cycle of the flea.
- The flea cycle is contained mainly within the home; pets pick up very few fleas from outside.
- Because fleas live mainly within the home and most houses are kept warm all year round, fleas are active throughout the year and not just in the summer.
- For each adult flea on your pet there will be at least 20 developing fleas in the carpets of your house, so your pet needs to be constantly protected against reification.
- The flea pupa, one of the developing stages of the flea, is resistant to any insecticide available for use in the home. It can survive for up to a year, so it can take a long time to rid a house of fleas.
Treatments Available
There are various forms of treatment, all available from your veterinary surgery. These come in the form of oral preparations, sprays, and spot-ons. There are also insecticidal shampoos available but these are not as effective as they do not leave residual protection once washed off.
House sprays can also be obtained from your vet and contain both an insecticide to kill any adult fleas in the carpet and also a flea hormone that prevents flea larvae from pupating. They need to be reapplied every 6 months.
Recommendations
The best form of flea control for you will depend on various factors including the type and number of pets you have. Remember, a single flea can start an infestation in your home and once established it may take up to a year to clear. It is much easier to prevent the problem arising by using constant flea control.
Discuss your requirements with your vet and he/she will explain in full the various options.
- Worms
Worms
There are two kinds of worms commonly seen in domestic dogs; namely roundworms and tapeworms.
Roundworms
These are the most commonly encountered worms in dogs, and all puppies will already be infested by the time they are born. As a general rule you will not know when your pet has roundworms as only the microscopic eggs are passed in the faeces, although occasionally an adult worm will be passed or brought up. In this case they appear as white, spaghetti like worms.
Tapeworms
Tapeworms are less commonly encountered and unlike roundworms puppies are not born with them. The most common species of tapeworm seen in dogs is actually spread when the animal swallows a flea or louse infected with the intermediate stage of the worm. Often if your pet gas tapeworms you will see segments which pass from the backend and are often found in the hair around the anus or on the floor where the animal has been sitting. They look like cooked rice grains and can often be seen to move.
Worming Your Dog
ROUNDWORMS - Puppies should be treated every 2 weeks until 12 weeks old then every month until 6 months old. Adults need routine treatment every 3-6 months.
TAPEWORMS - No treatment is required for the first 12 weeks of life. After this, treatment should be carried out whenever tapeworm segments are seen and at least once a year anyway.
There are several products available and your vet will be able to recommend the most suitable one for your dog. Do not use products bought from pet shops, as these are not as effective.
- Bloat - Gastric Dilation / Volvulus
Bloat - Gastric Dilation / Volvulus
Bloat is a most serious condition and mainly affects large deep chested breeds, it requires immediate veterinary treatment.
Description
The stomach becomes dilated due to an abnormal accumulation of gas/air. This 'enlargement' often results in a twisting of the gut. This then sets up a series of reactions within the body resulting in a critical condition which is frequently fatal. The series of events can take place very rapidly (within minutes). Bloat usually occurs after the age of 12 months. It can also affect puppies, but this is rare.
Causes
Many theories exist as to the causes of bloat, including:
Food Related
- Certain types of food, e.g. Soya based cereal foods
- Eating too quickly / eating too much at one meal
- Delays in the passage of food through the gut
- Presence of certain bacteria causing over fermentation
Physical
- Stress During showing
- Change of environment, e.g. kennelling
- Fear (thunderstorms / fireworks)
- Death of an owner or canine companion
- Males living with a bitch in season
- Illness
First Signs (roughly in order of appearance)
- Restlessness
- Unproductive vomiting / retching of a saliva type frothy substance which can resemble whisked egg white and/or bubbles (undigested food is usually not seen)
- IT IS NOW TIME TO CALL YOUR VET. EXPLAIN THAT YOU THINK YOUR DOG HAS BLOAT.
- Abdominal swelling
- Tightness over abdomen
- Stance -Dog stands with head down and legs apart
- Difficulty in breathing / shock followed by collapse
First Aid
You can give your dog 8 fluid ounces of an antacid. Brand names to look for are:
- Actonorm
- Altacite Plus
- Asilone
- Infacol
- Simeco
- Polycol
Ask the chemist for an activated type of antacid. Always keep one in the house and regularly check the expiry date.
Don't wait to see if the antacid improves your dog's condition. Get the dog to the Vet. Time is of the essence.
Not all vets agree with the administering of an antacid, so you should check this point with them. If you have given an antacid to your dog, remember to tell your vet which one adn how much.
Prevention
- Feed your dog at least twice a day to avoid stomach overloading
- Avoid your dog gulping down its food fast
- Avoid exercise for at least 1 hour before and 2 hours after a meal
- Do not feed before or after any situation that might cause your dog stress (for example, Dog Shows). If you withhold food on show day DO NOT feed your dog a large meal on returning home. Feed only half the quantity you would normally.
- Avoid excessive drinking at one time
- Avoid leaving your dog for long periods without being checked
- Get to know your dog's normal habits and you will recognise in good time when something is wrong
- Make sure your vet knows that your breed of dog is susceptible to bloat and talk to them about it. Ensure that your vet offers 24 hour cover and is close enough to your home in case of an emergency.
Treatment
As per your Veterinary Surgeon's instructions.
- Arthritis
Arthritis
Is Age Creeping Up on Your Dog?
As you know, dogs are naturally athletic and energetic animals, especially when they are young. However, this activity can eventually take it's toll. And it could mean that your dog is now suffering from wear and tear on his/her joints as a consequence. In fact many older dogs suffer from arthritis. (Vets consider all dogs over the age of seven to be older). Just as in Humans, arthritis is a condition where joints degenerate over time, often impairing mobility and causing pain. But unlike humans it is often more difficult to detect because dogs are much more stoical than we are and seldom complain. So what should you look out for?
Canine Arthritis
Although arthritis is usually associated with pain and stiffness in the joints, it is often only after the pain has been relieved, and your dog has renewed mobility, that you may come to realise just how stiff he/she had become. Lameness in one leg is usually fairly obvious, but if lameness affects more than one leg it may be much more difficult to recognise. Similarly, generalised stiffness, or stiffness when getting out of the basket in the morning or after exercise, may not be immediately obvious. Some dogs may not seem lame at all, showing only a mildly odd gait or lack of desire to go for walks.
What to Look For:
The four faces of chronic pain in dogs
Here are four simple questions that have been designed to help you recognise subtle changes in your dog's behaviour that could indicate pain:
1. Have you noticed a reduction in your dog's mobility?
- Difficulty in Jumping into car/chair or climbing stairs
- Limping or stiffness
- Difficulty in getting up
2. Have you noticed a reduction in your dog's activity?
- Reluctance to walk or play
- Sleeping/resting more, especially in one place
- Lethargy
3. Have you noticed changes in grooming habits?
- Unusual licking, sometimes leading to bald areas
- Chewing at joints
4. Have there been any changes in your dog's temperament?
- Less tolerant towards children and/or other dogs
- Reduced interaction with you /family
- Increased anxiety/clinginess
If you answer 'Yes' to any of the questions above, you should consult your Veterinary practice for advice and consider arranging a check-up for your dog.
- Canine Hip Dysplasia
It’s all in the hips - canine hip dysplasia
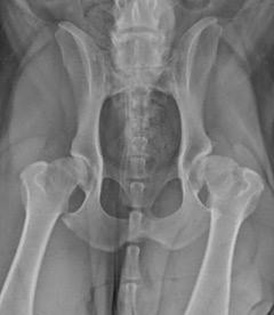 When compared to humans, dogs grow at an alarmingly quick rate, reaching almost full size before they are a year old. As giant and large breed dogs have such a short time to develop, they grow so rapidly that it can affect their joints and bones. This often results in life long disorders and causes them a lot of pain and discomfort. So let’s get the ball rolling with one condition we’re sure you’ve probably heard of: hip dysplasia!
When compared to humans, dogs grow at an alarmingly quick rate, reaching almost full size before they are a year old. As giant and large breed dogs have such a short time to develop, they grow so rapidly that it can affect their joints and bones. This often results in life long disorders and causes them a lot of pain and discomfort. So let’s get the ball rolling with one condition we’re sure you’ve probably heard of: hip dysplasia!Hip dysplasia is the most common developmental problem affecting the skeleton of dogs. As pups grow, the laxity of their hips (how well the head of the femur and the socket in the pelvis fit together) is the single most important risk factor for the development of arthritis. Loose hips develop arthritis quickly - the cartilage lining inside the joint gets eroded away, the capsule around the joint gets stretched and the head of the femur can start popping out of the socket.
This leads to the signs of hip dyplasia - some of which are: a rolling hip motion when walking, bunny hopping when running, not climbing the stairs at home, not wanting to play. All of these signs are uncomfortable for the pup and as things progress, will get downright painful.
What is hip dysplasia?
For anyone who can remember basic anatomy from school, the hip joint is made up of a ball and socket. Hip dysplasia occurs when the hip joints have not developed normally causing additional friction between the ball and socket. The deterioration of these joints can lead to osteoarthritis and loss of function in the hips.
Spot hip pain while they’re still young
Hip dysplasia in dogs is most frequently associated with large breeds such as German Shepherds, Labradors, Rottweilers and Labradoodles. However, it can affect small and medium dogs too.
It often begins while the dog is still young and physically immature, usually between the ages of 8 to 12 months old (however there are reports as early as 4 months in severe cases). It is always best to treat hip dysplasia before arthritis sets in; although it can be difficult to notice that your puppy is lame, particularly if both hips are affected.
How is hip dysplasia diagnosed?
Specialist orthopaedic vets can diagnose hip dysplasia in dogs quicker than most, particularly in young dogs showing less obvious symptoms. They will perform a thorough orthopaedic examination, and usually carry out x-rays or a CT scan.
How is hip dysplasia in dogs treated?
Hip dysplasia can be treated either surgically or medically.
For young dogs, there is a minimally invasive procedure called Juvenile Pubic Symphysiodesis (JPS). JPS involves fusing a small part of bone in the mid section of the pelvis, so that as the pup continues growing, the hip sockets rotate, keeping the head of the femur snug in the joint, stopping the erosion of the cartilage.
Pups with mild to moderate hip laxity are the ones that tend to benefit the most, and these pups are best identified by veterinary examination and PennHIP xrays to calculate their Distraction Index (which measures how loose their hips are).
Because the operation relies on the hip sockets rotating into place as the pup continues growing, the procedure needs to be performed at an early stage - for medium/large breeds by their 16th week (4 months old) and for giant breeds by the 20th week (5 months old) - to get the most benefit.
If left too late and arthritis has set in, other surgical procedures include a total hip replacement, which replaces the existing joint with an artificial one, or femoral head and neck excision which removes the head and neck of the femur bone.
If surgery is not an option, pain relief and anti-inflammatory drugs can be used to manage the pain from the arthritis. Swimming (hydrotherapy), physiotherapy and laser treatments are also great ways to alleviate discomfort.
Is your puppy at risk?
If your puppy is at high risk for developing hip dysplasia or you think they could be showing signs of joint pain, then have a chat with your usual vet about possibly seeing an orthopaedic specialist.
- Osteosarcoma (bone cancer): presentation & treatment options
Osteosarcoma (bone cancer)
By Sarah Mason, BSc BVSc PhD MRCVS
This presentation will discuss osteosarcoma, which is a cancer of the bones. It must commonly affects the long bones of the legs, but sometimes affects the jaw and other flat bones. I will talk about how cancer develops (pathogenesis), the signs your dog may show, diagnosis of osteosarcoma, treatment options and what kind of survival times and quality of life to expect.
Cancer occurs when cells in the body begin to divide uncontrollably. We do not know what causes this to happen, but several factors have been implicated in humans and in dogs. Genetics do play a part and certain breeds of dogs are more likely to develop certain types of cancer. Great Danes are one of the breeds that are more likely to develop osteosarcoma; a disease which most commonly affects large breed dogs.
Presentation
Osteosarcoma normally presents as lameness. Dogs initially are only mildly lame and this becomes worse over a period of weeks. In some animals an obvious swelling is noticed on the limb. Often the dog seems better with pain relief from the vet, but inevitably will deteriorate quite quickly. The most common places for osteosarcoma to occur are at the back legs above or below the knee, or the front legs, near the shoulder and ankle. Some dogs may seem to become suddenly lame and they can be in significant pain.
Diagnosis
X-rays can give us a very good idea to the dog has osteosarcoma, but a biopsy is required for definite diagnosis. Sometimes a diagnosis can be made on a needle biopsy, but other times a core biopsy is required. Frustratingly, sometimes biopsies are non-diagnostic and have to be repeated. Once the diagnosis is confirmed then we have to perform staging. This is when we determine if the tumour has spread or not. We take x-rays of the dog's chest to look for any nodules suspicious of tumour spread. We also normally ultrasound the abdomen and take samples from the local lymph node to check for any tumour cells and to make sure the dog does not have any other serious diseases.
Treatment Options
Treatment is amputation of the affected leg. This removes the primary tumour and also the source of pain. The dogs normally do very well once they've learned how to balance on three legs and will cope very well without the missing limb in most cases. The dog normally stays in hospital for a few days after surgery for pain relief and have the wound dressed. Unfortunately amputation does not cure the dog, as cancer cells will have already started to spread around the body and dogs will inevitably develop tumour spread, sometimes within months.
In order to minimise tumour spread we give chemotherapy with carboplatin, this slows down the rate of disease progression. Chemotherapy in dogs very rarely makes them sick, we use quite low doses of the drugs so that the dogs can stay at home and spend time with their family. They only have to come to the clinic every three weeks for 4 to 6 treatments.
Average survival times are 5 to 7 months with surgery only, and 7 to 11 months with surgery and chemotherapy. Some dogs will do better or worse than this and around 20% of affected dogs live for a year or longer. The cost of treatment for a Great Dane in a specialist hospital will be in the region of £1000-£1500 for staging, £1500-£2000 for surgery and £2000-£3500 for chemotherapy.
The main objective in treating pets with cancer is to ensure they have quality of life. This means they should be free of pain and be able to enjoy their normal daily activities. Alternative treatment for osteosarcoma consists of pain relief which can be tablets or syrups. We can also use palliative radiotherapy to relieve pain, or a drug called pamidronate which is given as a drip. If the dog had tumour spread at the time of diagnosis we would not proceed with surgery or chemotherapy in normal circumstances because unfortunately the survival time once this has occurred is only weeks to months.
Outcome
While osteosarcoma is an aggressive disease, we can achieve good quality of life in most patients for around 5 to 12 months. While six months may not sound like a long time, it is 10% of a six-year-old dog's life and the owners of most dogs who have amputation and chemotherapy for osteosarcoma are usually happy that they had the treatment.
- Cardiomyopathy
Cardiomyopathy
Can we fix a broken heart? Dilated Cardiomyopathy in the Great Dane
Hannah Stevenson BVMS (Hons) CertSAM MRCVS
We have known for some time that dilated cardiomyopathy occurs with increased frequency in the Great Dane in comparison to some other dog breeds. Despite this, there has been very little research into this disease in Great Danes. We have been screening dogs at the University of Liverpool for the last three years, and we're starting to build up a better picture of DCM in the UK population. This started with the LUPA project, which is still aiming to identify the genetic mutation responsible for DCM in a number of dog breeds. We have also received funding from the Breed Council and the Kennel Club to continue this research. This talk will aim to summarise the main characteristics of DCM in all dogs, and discuss some of the findings of our research so far.
The normal heart
The heart is one of the most important organs in the body. It consists of four main chambers, the atria (or receiving chambers) and the ventricles (or pumping chambers). The left side of the heart pumps blood around the body, and the right side of the heart pumps blood to the lungs, where the blood picks up oxygen. Normal heart function is required for nutrients and oxygen to be delivered to the tissues of the body, and for waste products to be removed.
Dilated Cardiomyopathy
Dilated cardiomyopathy is a disease of the heart muscle which affects a number of large and giant breed dogs, people, cattle, hamsters and even turkeys! The disease is characterised by:
1. Dilation and rounding of the heart chambers (particularly the left ventricle and the left atrium)
2. Impaired pumping ability (contractility) of the heart
3. Thinning of the heart muscle
Ultimately the donated and poorly contractile heart is unable to pump blood efficiently around the body. There is a very long phase when a dog will show no clinical signs of heart dysfunction, or may show any very mild signs (such as slowing at exercise, or taking longer to recover from exercise than normal). This phase is the preclinical phase of DCM.
Dilated cardiomyopathy is usually an adult-onset disease, so dogs often do not show signs until they are older. In our experience, most great Danes show signs from 6 years or older, with some not developing any signs until 8 or 9 years of age or older. Some never show signs of having the disease at all, and may die of other diseases.
The most commonly reported signs of DCM in Great Danes are those of congestive heart failure. Congestive heart failure occurs when there is pressure in the chambers of the heart, and blood 'backs up' in the lungs or in the blood vessels of the body. The high pressure inside the vessels causes fluid to leak out into the surrounding tissue. In DCM, left-sided heart failure is more common, where fluid builds up in the lungs. This is called pulmonary oedema. Dogs with congestive heart failure will show signs of severe exercise intolerance, cough or difficulty breathing.
Inheritance of DCM
A group of researchers in the USA have published pedigrees of dogs, suggesting that the inheritance of DCM in Great Danes is X-linked recessive. This would mean that male dogs were much more likely to develop the disease (see genetics notes). We are not sure if this is the case in the UK.
In other dog breeds (Dobermans, Newfoundlands) the disease is thought to be autosomal dominant – it appears in every generation of the pedigree and an equal numbers of male and female dogs. Clearly, the advice regarding breeding of dogs with DCM varies greatly depending on how the disease is inherited. This is one of the most important things to establish in our population of dogs, even before a genetic test becomes available.
The LUPA project is currently running tests on samples collected here in the UK and in the rest of the world, to try and determine the genetic mutation or mutations responsible for DCM in Great Danes. These are in the early stages, but we are hopeful that we have found a significant locus.
DCM in UK Danes
We have they screened ever 100 Great Danes as part of our research. In most cases these dogs have been presumed healthy by their owners and were being screened as normal dogs. We have identified approximately 20% of the dogs screened as having DCM. This is a worryingly high prevalence. Most dogs have been 6 or older, but some of the more recent dogs have been younger (disease identified in dogs as young as 4). A number of dogs are coming back for repeat scans each year, which is giving us vital information on the progression of the disease.
The other vital information that we gain by screening Great Danes over time is that we build up a picture of what is normal for Danes on heart scans. For example, some of the measures of contractility that are published for dogs in general do not always hold true for Great Danes, and they may have slightly abnormal contractility that is of no clinical significance. We have also found differences in the normal values for male and female Great Danes.
Sudden death in great Danes
Sudden death occurs in other breeds that develop dilated cardiomyopathy, particularly in Dobermans. In this breed, dogs can develop ventricular arrhythmias, or more 'classical' DCM with heart failure, or both. Some Dogstar I suddenly at teenagers without ever having shown signs of the disease. Sudden death and heart failure due to DCM can occur in the same families, and there are differences between males and females in the development of disease.
Sudden death is a problem that we have recently started investigating in more detail, as there were increasing reports of this problem in UK Danes. The Breed Council recently purchased a Holter monitor (ECG recorder), which is giving us vital information about ventricular arrhythmias which we think may be the underlying cause of many sudden death cases. The Holter records an ECG for 24 hours, and we can therefore identify the number and severity of ventricular arrhythmias. A normal dog should have fewer than 20 extra beats (VPCs) in 24 hours. Anything over 100 VPCs in in 24 hours is considered abnormal and we often recommend treatment when there is over 1000 VPCs in 24 hours.
We have also received hearts from dogs that have died suddenly. This is absolutely vital to our research and we are so grateful to everyone that has contributed.
Can we fix a broken heart?
Unfortunately, dilated cardiomyopathy is an incurable disease, but we can give dogs medication to prolong their life, and improve their quality of life. Once the dog is in heart failure, there are numerous medications that may be of benefit. It is likely your dog will be prescribed:
1. A diuretic (e.g. furosemide) to reduce fluid buildup in the tissues
2. An ACE-inhibitor (e.g. Fortekor, Vasotop) to reduce salt and water retention that occurs in heart failure, and to dilate the blood vessels, reducing the work the heart has to do
3. Vetmedin to improve the pumping ability of the heart
Other drugs that you may receive include Prilactone (a drug that reduces scar tissue in the heart), or drugs to control abnormal heart rhythms such as digoxin or diltiazem.
We now have evidence from a study in Dobermans and a lot of evidence from people that giving a dog an ACE-inhibitor BEFORE it develops clinical signs of disease can prolong the time to onset of clinical signs. We therefore now suggest that this treatment is given to any dog with preclinical DCM.
If a dog is identified as having ventricular arrhythmias, we can give medications to try and reduce the number of arrhythmias that they are having. Most often we use a drug called sotalol. We hope that these drugs will reduce the likelihood that the dog will die suddenly of their arrhythmias, but definite evidence for this effect is lacking.
Ultimately, reducing the number of dogs developing DCM will be the best way of controlling the disease. We faced numerous, peculiar changes when trying to reduce the instance of DCM in Danes. Firstly, at the moment, we cannot test for the disease in young dogs, and therefore animals may be bred from before a diagnosis is made. Furthermore, we do not yet definitively know the mode of inheritance of the disease, and further research is needed to investigate whether dogs with ventricular arrhythmias, and dogs with DCM, have the same disease. In addition, some dogs may die of other causes before they ever show signs of the disease, and therefore may be considered to be 'normal' if they never had a heart scan.
Myself and all of my colleagues involved in DCM research are very grateful to everyone who has participated in a study so far, and urge more people to bring dogs for screening – remember, the age limit is now only 4 years old! We hope to be using the Holter monitor much more in the future, as well. Any information you can provide about dogs with sudden death or DCM will always be appreciated and will help further our understanding of this disease in Danes.
If you have any questions, or want to be involved in the research, contact me on (0151) 795 6100 or hmc79@liv.ac.uk.
- Lungworm - is your dog at risk?
Lungworm - is your dog at risk?
Did you know that the lungworm parasite A. vasorum can be found in slugs, smails and even frogs that you find in your garden?
Read this Bayer HealthCare leaflet on Lungworm for more information.
(PDF, 2.2MB) - Neutering and Spaying
Neutering and Spaying
Why Should I Have My Pet Neutered or Spayed?
One of the many decisions facing pet owners is whether or not to have their pet neutered (or spayed as it is referred to in females).
The most obvious reason is to prevent unwanted pregnancies, but there are several other behavioural and health reasons too which are explained here.
Spaying Female Dogs
Un-spayed female dogs (bitches) usually come into season (heat) twice a year. Seasons may last for up to a month, and during this time they are very attractive to male dogs and can become pregnant. To avoid unwanted pregnancies, they have to be kept away from male dogs, which can be difficult as their natural urge will be to go to them.
Although seasons can be controlled by other means, spaying provides excellent long term control. Having been spayed your dog won't come into season and therefore won't have to suffer the associated frustrations or experience phantom pregnancies. Better still, she will be able to enjoy her walks all year round!
Spaying also removes the possibility of pyometras (life-threatening uterine infections) and reduces the occurrence of mammary tumours later on in life.
Unless you intend to breed from your dog, we normally recommend that she is spayed at 6 months of age, or 12 weeks after her first season depending on the breed. Your vet will be able to advise you on the correct timing for your dog.
Traditional spaying (for females) is a routine operation where the uterus and the ovaries are removed. However, we shouldn't lose sight of the fact that, for dogs in particular, it is major abdominal surgery.
For this reason, in addition to traditional spaying, a bitch can be spayed by Keyhole Surgery (laparoscopy) - the gentle way to spay your female dog.
Highcroft Veterinary Group is very proud to be one of the first veterinary practices in the country to offer clients the option of a laparoscopic, or "keyhole", bitch spay for their pet.
Whilst there is conventional spaying, laparoscopy is a safer, less invasive method of surgery that will give your pet much smaller wounds, less post operative pain and discomfort and a quicker recovery.
Although it is still very rare in the veterinary field, keyhole surgery is relatively commonplace in human hospitals and has replaced many of the more invasive surgical procedures - if you have experienced keyhole surgery yourself you will be well aware of the benefits!
In conventional or open surgery a large incision is made to allow the surgeon to locate and perform an operation on the part of the body that needs the surgery. Unfortunately this usually involves a certain amount of pulling and tugging in order to allow good visualisation and handling.
However with keyhole surgery very small holes are made through the skin and muscles into the body (usually around 5mm diameter) through which a camera and long, slender, surgical instruments can be introduced to perform the surgery inside the body with maximum precision and minimal invasion.
The surgeon has excellent visualisation through the camera during the operation and can be certain that there are no complications before the wounds are stitched.
In a conventional spay both the uterus and the ovaries are removed (ovariohysterectomy) and, although this is an everyday procedure, it is major surgery, as anyone who has had a hysterectomy will know!
A keyhole spay is far less traumatic and only the ovaries are removed (ovariectomy).
There is no difference in the effect of the two operations and both techniques will stop the bitch from coming into season (what's more the uterine disease pyometra is still avoided as ovaries are required to contract the disease).
Not surprisingly, keyhole surgery is more expensive than conventional surgery as it requires very specialist equipment and highly skilled surgeons.
Neutering Male Dogs
The main reason for neutering a male dog is to prevent unwanted puppies. However it can also help to control inappropriate behaviour, and a neutered dog is almost always much more docile and affectionate.
Neutering controls excessive sexual drive and reduces inappropriate sexual behaviour. It also reduces testosterone driven behaviour such as scent marking, straying (particularly when a local bitch comes into season!) and hostility towards other dogs (particularly males), and towards people.
Another important benefit of neutering is that it reduces some of the health problems that can happen later on such as prostrate gland problems and testicular cancer.
As a general rule, unless you want to breed from your dog, we recommend that you have him neutered as early as possible, usually at around 6 months of age, before any inappropriate sexually related behaviour sets in.
The neutering operation (for males) is straightforward and involves removing the testicles under anaesthetic.
- Pet Blood Bank UK
Pet Blood Bank UK
Launched in 2007, Pet Blood Bank UK is the first and only charity of its kind that provides a canine blood bank service for all veterinary practitioners across the UK.
www.petbloodbankuk.org

